Home / Onlay vs. Crown
Onlay vs. Crown: How Philadelphia Dentists Decide Which One You Need
The difference between an onlay and a crown comes down to one question: how much of your tooth is still healthy? An onlay covers only the damaged portion — the cusps and biting surface — while a crown encases the entire visible tooth down to the gumline. Neither is universally better. The right choice depends on what’s left of your natural tooth structure.
At Razavi Dental in Philadelphia, Dr. Leily Razavi evaluates each tooth individually before recommending either restoration. Here’s how that decision gets made.
What Is an Onlay?
An onlay — sometimes called a partial crown — is a custom-fitted restoration that covers one or more cusps of a damaged tooth without removing healthy enamel around the sides. It bonds directly to the remaining tooth structure and is typically made from porcelain, ceramic, or gold.
Onlays are appropriate when:
- Decay or a crack affects one or more cusps but the walls of the tooth are intact
- An old filling has failed but surrounding enamel is still strong
- Preserving as much natural tooth as possible is the priority
Because onlays remove only the damaged area, roughly 60–75% of your natural tooth structure is preserved — compared to 25–40% with a crown.
What Is a Partial Crown? (And How Is It Different From a Full Crown?)
“Partial crown” is simply another name for an onlay. The terms are used interchangeably — your dentist may use either depending on how they were trained or how they prefer to explain it to patients. If you’ve been told you need a partial crown, you’re being offered an onlay.
The distinction from a full crown is exactly what it sounds like. A partial crown covers only the damaged portion of the tooth — typically one or more cusps and the biting surface. A full crown encases the entire visible tooth down to the gumline. Everything else about the two restorations — materials, lab fabrication, two-appointment process, bonding — is essentially the same.
For the purposes of this page: onlay, partial crown, and partial coverage restoration all refer to the same thing.
A crown is a full-coverage cap that fits over the entire visible portion of a tooth. It’s the right choice when the tooth is too compromised to support a partial restoration.
Crowns are typically recommended when:
- More than 50% of the tooth structure is decayed or missing
- The tooth has undergone root canal therapy
- Cracks extend below the gumline
- Multiple surfaces are damaged
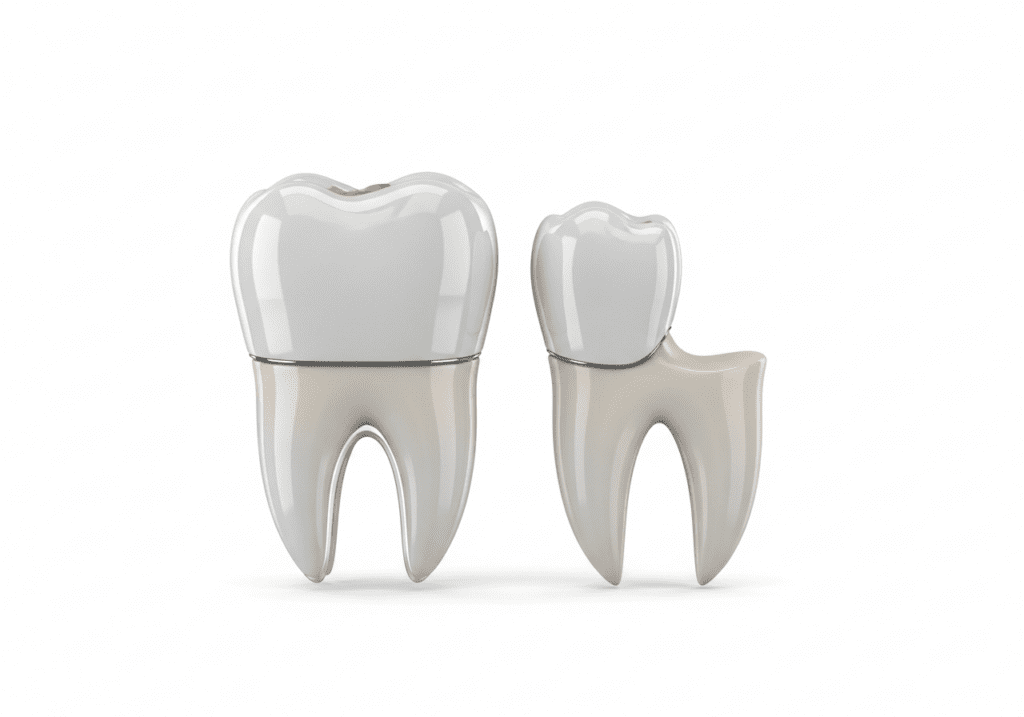
Left: full crown. Right: partial onlay coverage.
Crowns are also the standard restoration after root canals on back teeth, where chewing forces are highest and an unprotected tooth is at serious risk of vertical fracture.
Onlay vs. Crown — Direct Comparison
| Onlay | Crown | |
|---|---|---|
| Coverage | Partial (cusps and biting surface) | Full (entire visible tooth) |
| Tooth preserved | ~60–75% | ~25–40% |
| Best for | Moderate damage, intact walls | Severe damage, post-root canal |
| Avg. cost (Philadelphia) | $800–$1,300 | $1,100–$1,700 |
| Sensitivity after | 3–7 days typical | 7–14 days typical |
| Longevity | 12–18 years average | 12–18 years average |
| Future options | Can upgrade to crown later | Limited if it fails |
For a direct comparison of crowns and veneers for cosmetic cases, see our crown vs veneer guide.
Onlay vs. Crown: Why Don't More Dentists Offer Onlays?
Onlays require more precision than crowns. The preparation is more technically demanding, the margins are harder to achieve, and bonding an onlay correctly takes more time and skill than placing a crown. Some dentists default to crowns because the procedure is more standardized and insurance reimbursement is more predictable.
That doesn’t mean a crown is always the right call. When enough healthy tooth remains, an onlay is the more conservative and often preferable choice — it preserves your natural tooth, reduces the risk of nerve irritation, and keeps your options open for future treatment if something goes wrong down the road.
At Razavi Dental, we recommend onlays when the clinical situation supports them, not based on what’s simpler to place.
Onlay for a Cracked Tooth — Does It Work?
It depends on where the crack is and how deep it runs.
An onlay is appropriate for a cracked cusp when the crack is confined to the chewing surface and hasn’t propagated below the gumline or into the root. The onlay covers and stabilizes the cracked area, bonding to the remaining tooth structure and preventing the crack from spreading under normal chewing forces.
An onlay is not appropriate when the crack extends below the gumline, runs through multiple surfaces, or reaches the pulp. In those cases a crown is the minimum intervention — and depending on crack depth, a root canal may also be necessary before any permanent restoration is placed.
Cracks aren’t always fully visible on x-rays. Your dentist may use bite testing or transillumination to map the crack before deciding between an onlay and a crown. If there’s genuine doubt about crack depth, the safer clinical choice is a crown — not because onlays can’t work on cracked teeth, but because an onlay that fails due to an underestimated crack means starting over with less tooth remaining.
Onlay vs. Crown After a Root Canal
After a root canal on a back tooth, a crown is almost always the right call.
Root canal therapy removes the pulp — the nerve and blood supply — from inside the tooth. Over time, a tooth without its internal blood supply dehydrates and becomes brittle. Back teeth absorb the majority of chewing force. A brittle tooth under that load is at serious risk for a vertical root fracture, which typically means extraction.
A crown encases the entire tooth and distributes those forces across the restoration rather than concentrating them on weakened structure. This is why crowns after root canals on posterior teeth are considered standard of care.
Where an onlay can be considered after a root canal: on front teeth, which bear significantly less bite force. This is a case-by-case clinical decision based on how much structure remains and what the aesthetic goals are.
If you’ve had a root canal on a back tooth and don’t yet have a permanent crown, don’t wait. The temporary filling placed after the root canal isn’t designed for long-term use, and an unprotected tooth is vulnerable to fracture and reinfection.
What Material Should Your Onlay or Crown Be Made From?
Material choice affects how long your restoration lasts, how it looks, and how it holds up under the specific forces in your mouth.
Porcelain and ceramic
The most common choices for onlays on visible teeth. They match natural tooth color closely, bond well to enamel, and hold up well under normal chewing forces. A good choice for premolars and teeth in the smile zone.

Zirconia
The strongest ceramic option available. It resists fracture better than porcelain and handles heavy grinding forces on back molars. If you clench or grind your teeth, zirconia is worth the conversation. Aesthetics are slightly less natural than porcelain but close enough for most back teeth.
Gold alloy
The longest-lasting option — gold onlays and crowns from 20+ years ago are still functioning in patients’ mouths today. Gold is biocompatible, gentle on opposing teeth, and fits with exceptional precision. Back molars only, for obvious reasons.
Composite resin
Less expensive but also less durable — typically 5–10 years versus 15+ for ceramic or gold. At Razavi Dental, composite onlays are occasionally used as a transitional restoration but not as a long-term solution for primary chewing teeth.
The Gray Area — When Either Could Work
The clearest cases are straightforward: a cracked molar with intact walls gets an onlay; a tooth that just had a root canal gets a crown. But many cases fall in between.
Large failing filling, walls still present. A molar with a failing silver filling showing recurrent decay around its edges is a classic gray-area case. If the walls are structurally sound, an onlay replaces the old filling and restores the chewing surface. If the walls have thinned or hairline cracks are visible on x-ray, a crown is more predictable. Both could succeed — the decision comes down to wall integrity.
Hairline crack, no symptoms. A crack that hasn’t reached the root and isn’t causing pain could reasonably be treated with either. An onlay covers the damaged cusp and reinforces it. A crown prevents the crack from propagating in any direction. If the crack is isolated to one cusp, an onlay is often the first approach. If it runs across multiple cusps, a crown is safer.
Large cavity, root canal not yet needed. When decay is extensive but the nerve is still healthy, an onlay preserves the nerve by minimizing drilling. A crown requires removing more healthy enamel, which increases the statistical chance the nerve will eventually need treatment. This is one of the strongest clinical arguments for choosing an onlay when the situation allows.
If you’re in a gray-area situation, ask your dentist directly: what happens if we do the more conservative option and it’s not enough? A clear answer tells you what you need to know.
Patient Scenarios — Matching the Situation to the Restoration
Moderate decay on one cusp. The tooth has never had a root canal, walls feel solid, no cracks visible on x-ray. Textbook onlay candidate.
Root canal on a lower molar five years ago, still has the temporary filling from the procedure. High risk for vertical fracture. Crown — and it’s overdue.

Scenario 3
Old silver filling taking up most of the chewing surface of a premolar, intact but deep, new crack in one cusp. If walls are solid, onlay. If walls have been undermined by the large filling, crown.
Scenario 4
Planning a smile makeover — changing shape, size, or color of multiple teeth. Crowns offer complete control over the final appearance. Onlays blend with existing tooth color, which works for single-tooth restorations but is a limitation when the goal is full transformation.
Onlay Procedure — What to Expect
An onlay takes two appointments, typically 2–3 weeks apart.
First appointment (60–90 minutes)
Your dentist removes the decay or damaged tooth structure, shapes the area to receive the onlay, and takes a digital scan or impression. A temporary covering protects the tooth while your permanent onlay is fabricated at the lab.
Between appointments (10–14 days)
The lab mills your onlay from the selected material. Porcelain and zirconia are the most common choices for back teeth.
Second appointment (45–60 minutes)
The temporary is removed, the permanent onlay is checked for fit and bite, then bonded to your tooth with adhesive cement.
Onlay Recovery Time
Most patients have mild sensitivity to temperature for 3–7 days after an onlay is placed. Over-the-counter pain relievers are usually enough. You can eat normally after the anesthesia wears off, though it’s wise to avoid very hard or sticky foods for the first 24–48 hours. By the end of the first week the tooth should feel close to natural.
Call if you experience sharp pain when biting, sensitivity that’s getting worse instead of better, or if the bite feels off — those are signs the onlay may need a simple adjustment.
Can You Eat Normally With an Onlay?
Yes. Once an onlay is permanently bonded it functions like a natural tooth. You can eat normally, including firm and crunchy foods, with the same care you’d use with any restored tooth. Avoid chewing ice, biting hard candy directly, or using your teeth to open packages — those habits damage natural teeth and restorations equally.
If you grind your teeth at night, a custom nightguard is strongly recommended. Grinding generates forces well beyond normal chewing and is one of the primary reasons onlays and crowns fail early.
Does Insurance Cover Onlays?
The onlay vs crown insurance question comes up often. Most PPO dental plans cover onlays at the same benefit level as crowns — typically 50% after your deductible, subject to your annual maximum. Some plans classify onlays as a major restorative procedure with a waiting period, or pay at the crown benefit rate and require you to cover the difference.
Inlays are sometimes excluded or covered at a lower rate because some insurers classify them closer to a filling than a crown. This varies by plan — always verify your benefits before treatment.
Our front desk will check your coverage before your appointment so there are no surprises.
How Long Do Onlays and Crowns Last?
The onlay vs crown longevity question is simpler than most patients expect — both last an average of 12–18 years. Studies show properly placed onlays have survival rates comparable to crowns at 10 years. The American Dental Association recommends the same maintenance for both — twice daily brushing, daily flossing, and regular cleanings. Gold onlays often last 20+ years. Porcelain and zirconia are close behind when the bite is well-managed.
What affects longevity more than the restoration type: oral hygiene, whether you grind your teeth, and whether you keep regular cleanings. Recurrent decay at the margin is the most common reason either needs to be replaced.
Frequently Asked Questions About Onlay vs Crown
What is the difference between an inlay and an onlay?
An inlay sits inside the tooth between the cusps. An onlay extends over one or more cusps. If the cusps themselves are damaged, you need an onlay. In practice, onlays are more common because by the time a tooth needs an indirect restoration, the cusps are usually involved.
Is "partial crown" the same thing as an onlay?
Yes. Same restoration, different name. Some dentists use “partial crown” because patients already understand what a crown is — calling it partial communicates immediately that it’s more conservative. If your dentist recommends a partial crown, they’re recommending an onlay.
Can an onlay fix a tooth that already has a filling?
Yes. If you have an old silver filling that’s failing — decay around the edges, cracks starting to form in the surrounding tooth — and the walls are still solid, an onlay is usually the right replacement. The old filling and any new decay come out, and the onlay restores the chewing surface without prepping the entire tooth for a crown.
Can an onlay be replaced with a crown later?
Yes. Because onlays preserve more tooth structure, there’s almost always enough remaining to place a crown if the onlay fails years down the road. This is one of the practical advantages of starting with the more conservative option.
My dentist recommended a crown. Should I get a second opinion?
If you’re unsure, a second opinion is always reasonable for any major restoration. Ask specifically whether an onlay was considered and why a crown was recommended instead. A dentist who can clearly explain the clinical reasoning — wall integrity, crack depth, percentage of structure remaining — is giving you what you need to make a confident decision.
Does a crown always follow a root canal?
On back teeth, yes — almost always. Back teeth absorb the majority of chewing force, and a tooth without its internal blood supply becomes brittle over time. A crown prevents the vertical fractures that can make a tooth unrestorable. On front teeth, which bear less force, a crown isn’t always required after a root canal, though it’s often still recommended.
How soon after getting an onlay can I eat?
After the anesthesia wears off — typically 2–4 hours. Use some caution with very hard foods for the first 24–48 hours. By day three most patients report the tooth feels close to natural.
Schedule an Evaluation at Razavi Dental
If you’ve been told you need a crown, or you have a failing filling or cracked tooth and want to understand your options, Dr. Razavi can evaluate whether an onlay is appropriate for your specific situation.
